An Examination of the Lowest-Rated Long Term Care Facilities Participating in New Jersey’s Medicaid Program
- Posted on - 02/2/2022
Table of Contents
Executive Summary
This report identifies New Jersey’s residential long-term care facilities (LTCs) — also known as nursing homes[1] — that consistently receive the lowest possible rating and addresses how the New Jersey Medicaid program (Medicaid) continues to provide substantial funds to these LTCs despite their longstanding failure to improve the safety and quality of their care. Continued funding of these facilities without consideration of their longstanding low ratings exposes Medicaid beneficiaries to unnecessary risks and results in taxpayer funds being used for care that is substantially below average.
Based on public data from the U.S. Department of Human Services, Centers for Medicare & Medicaid Services (CMS), the Office of the State Comptroller (OSC) found that New Jersey’s 15 lowest-rated LTCs, which consist of LTCs that have received the lowest CMS overall rating (one-star) in the first month of each quarter for six of the past eight quarters in 2020 and 2021, provide services to approximately 1,850 Medicaid beneficiaries, or 6.5% of the 28,500 Medicaid beneficiaries residing in New Jersey LTCs.[2] The Medicaid program annually pays these facilities an average of $103 million. In total, the Medicaid program annually spends around $1.74 billion for LTC services, which comprises about 12% of the annual Medicaid budget. [3]
During the period we examined, from 2013 to 2021, the lowest-rated LTCs provided care for Medicaid beneficiaries and received substantial government funding, while consistently receiving the lowest ratings for health inspections, quality measures, and staffing rates. This means that every day thousands of Medicaid beneficiaries have lived in and received health care from LTCs that have been repeatedly cited by state inspectors for serious, widespread, and uncorrected deficiencies that placed patients at great risk of harm. Because Medicaid funds follow Medicaid beneficiaries — and the State’s recent effort to incentivize higher quality care thus far has failed to distinguish in a meaningful way between the highest and lowest rated facilities — the State has paid the lowest-rated LTCs at virtually the same rate as it paid higher-rated LTCs.
This report recommends changes to New Jersey’s Medicaid program to require one-star LTCs to improve their quality of care if they want to remain in the Medicaid program, with a goal of aligning Medicaid payments with improved LTC performance. OSC recommends that the Department of Human Services (DHS), Division of Medical Assistance and Health Services (DMAHS), with support from the Department of Health (DOH), institute a phased approach through which DMAHS imposes increasing levels of restriction on these LTCs while affording the LTCs an opportunity to improve their ratings before the most severe restrictions are imposed. If the LTCs do not improve, DMAHS may bar them from participating in the Medicaid program. In the absence of some consequence for their continued low ratings, the lowest-rated LTCs, some of which have had low ratings for many years, appear unlikely to improve the conditions and care in their facilities. The recommendations in this report, if implemented, will complement and supplement the various legislative and regulatory reforms that DOH and DHS are implementing.
As part of OSC’s oversight of the Medicaid program, and as a way to evaluate any changes that are implemented, OSC periodically will update the findings contained in this report, including the list of LTCs that consistently receive the lowest possible CMS rating, through OSC’s LTC Dashboard.
Background
OSC is an independent agency responsible for monitoring and auditing government programs and agencies, reviewing the efficiency and effectiveness of government functions and programs, identifying cost savings, preventing misconduct within the programs and operations of government agencies, and investigating fraud, waste, and abuse. The State Comptroller is charged with implementing the Medicaid Program Integrity and Protection Act, N.J.S.A. 30:4D-53 to -64, by, among other things, ensuring that the State spends its Medicaid resources in a responsible and effective manner. OSC performs these duties through its Medicaid Fraud Division.
Medicaid is a joint federal and state program administered by states. In New Jersey, DMAHS administers the Medicaid program. DMAHS provides health insurance for approximately 2 million residents, including residents who are aged, blind, disabled, and low- and moderate-income.[4] In state fiscal year 2019, the Legislature budgeted more than $14 billion in state and federal funds to New Jersey’s Medicaid program.[5]
DOH serves as the state regulatory agency for LTCs. It licenses and oversees the enforcement of regulations for LTCs in New Jersey. DOH employees serve as federal contractors for CMS, performing LTC inspections for CMS. For these inspections, DOH reports its survey findings to CMS, which incorporates these findings into its rating assessment tool to determine LTC ratings. DOH maintains reports of the federal surveys on its website. Separately, DOH has its own statutory authority to license and inspect LTCs, investigate potential noncompliance, demand corrective/remedial actions, impose penalties, and take other enforcement steps.
OSC shared a draft of this report with DOH and DHS. OSC considered comments received from those entities prior to issuing this report. In addition, in developing this report, OSC obtained valuable guidance from the New Jersey Office of the Long Term Care Ombudsman, a state agency charged with monitoring and advocating with regard to the adequacy of the care received, and the quality of life experienced, by residents of health care facilities in New Jersey, including LTCs.
Findings
A. New Jersey’s lowest-rated LTCs consistently have performed poorly for many years.
State and federal inspectors regularly inspect New Jersey’s LTCs and provide their findings to CMS. The data that results from those inspections allows CMS to compare the quality of LTCs over multiple years, using a one to five-star rating system, with one-star being the lowest and five-stars the highest. CMS compiles this information in its Care Compare website.[6]
1. CMS Ratings
The linchpin of the CMS rating system is the health-inspection score. This score is developed based on unannounced site visits conducted by a team of state surveyor healthcare professionals who spend several days in the LTC assessing a variety of practices and policies in such areas as resident rights, quality of life, medication management, skin care, resident assessment, nursing home administration, environment, and kitchen/food services. After CMS establishes an LTC’s health-inspection score, it adds or subtracts points based on the LTC’s quality and staffing measure scores to arrive at an aggregated score. For an LTC to be among the lowest performers for the first month of each quarter for at least six of the past eight quarters means that the LTC consistently has had more widespread, serious, and uncorrected deficiencies than LTCs with higher star ratings.
The CMS rating system is a nationally recognized and accepted measure of LTC performance. As with any rating system, it cannot predict a resident’s level of satisfaction in a particular facility or future outcomes at a specific facility. It does provide, however, meaningful information about the areas it measures. For example, an analysis of CMS rating data found that one-star nursing homes are more than 400 times as likely to have an actual harm citation on their most recent survey (or in the past 12 months of substantiated complaints) than five-star nursing homes. Specifically, 45.2% of one-star nursing homes have had such a citation, compared to 0.1% of five-star nursing homes. Moreover, that same report found that no five-star nursing homes had an immediate jeopardy citation — on either of its two most recent surveys — and none had a substandard quality of care deficiency on the most current survey, while approximately one-fifth of one-star nursing homes had each of these dangerous health-inspection findings. Accordingly, the data shows that, on average, it is far more likely that a person receiving care in one of the lowest-rated LTCs is at a higher risk of harm than a person receiving care at a five-star rated LTC.
The three CMS measures used to form the overall score — health inspections, quality, and staffing — are comprised of the following elements:
- Health Inspections — State inspectors conduct yearly health and safety inspections of nursing homes for compliance with Medicare and Medicaid regulations. An LTC may also be inspected based on a complaint submitted by a resident (or other individual) or based on a facility's self-reported incident. LTCs are also inspected for compliance with infection control and prevention standards. CMS bases the health-inspection score on deficiencies found in the three most recent health inspections and on any complaint, incident or infection control investigations over the last three years. CMS assigns points based on the scope and severity of the health-inspection findings, with more serious, widespread deficiencies receiving more points and additional points assigned for substandard quality of care. Deficiencies that the LTC fails to address receive additional weight, which leads to higher point totals. The top 10% of LTCs in a state receive five-stars, the middle 70% receive two, three, or four-stars, and the bottom 20% receive one-star. DOH has regulatory authority over LTCs in the state and acts as both the federal and state survey agency, performing inspections and investigations of LTCs.
- Quality Measures — This rating measures LTC care quality, broken down between outcomes for short-term stay residents and long-term stay residents. The measures include the percentage of residents who have pressure ulcers (bed sores), received flu and pneumococcal vaccinations, received an antipsychotic medication, experienced one or more falls with major injury, have symptoms of depression, and are losing too much weight. CMS applies clinical and claims data reported by the LTCs to clinical quality measures to determine each LTC’s score.
- Staffing — The staffing rating is based on Registered Nurse (RN) hours per resident per day, total nurse staffing (including RN, licensed practical nurse (LPN), and certified nurse aide (CNA) hours per resident per day). These staffing hours include both staff employed by the LTC and staff supplied through an agency or individual contract with the LTC. Staffing hours of different types of staff are calculated using payroll and resident census data submitted by LTCs to CMS.
As part of the health-inspection process, a finding of “immediate jeopardy” is a serious deficiency. According to DOH, immediate jeopardy describes “a situation in which immediate corrective action is necessary because the facility’s noncompliance with one or more requirements of participation has caused, or is likely to cause, serious injury, harm, impairment, or death to a resident receiving care in a facility.” Examples of circumstances that led to an immediate jeopardy finding include, for instance, the following as reported in public records maintained by DOH:
- An LTC staff member caused a resident to fall out of a wheelchair and another staff member roughly pulled the resident back into the wheelchair. After returning to his room, the resident complained of pain. The LTC transported the resident to a hospital where the resident was admitted for injuries suffered at the LTC and the LTC failed to investigate or report this incident for five days.
- An LTC failed to monitor a resident with dementia and allowed the resident to wander off premises. The resident was found hours later near a busy roadway.
As noted, such conditions are far more likely found in the LTCs with one-star ratings than those with a five-star rating.
2. Ratings for New Jersey’s LTCs
OSC reviewed aggregated LTC ratings compiled by CMS.[i] The overall average rating for LTCs in New Jersey is 3.6 stars, which exceeds the national average of 3.1.
OSC examined CMS data from 2013 to 2021, with particular focus on data for 2020 to 2021 to assess whether New Jersey LTCs that accept Medicaid beneficiaries performed poorly over an extended number of years. That analysis revealed that one in fourteen of New Jersey’s 339 LTCs recently received the lowest ratings and that more than half of those LTCs experienced a sustained period of low ratings. The chart below sets forth New Jersey LTCs by each rating category (1 – 5-stars).
Exhibit A
Number of LTCs with NJ Medicaid Beneficiaries by Overall Rating as of October 2021
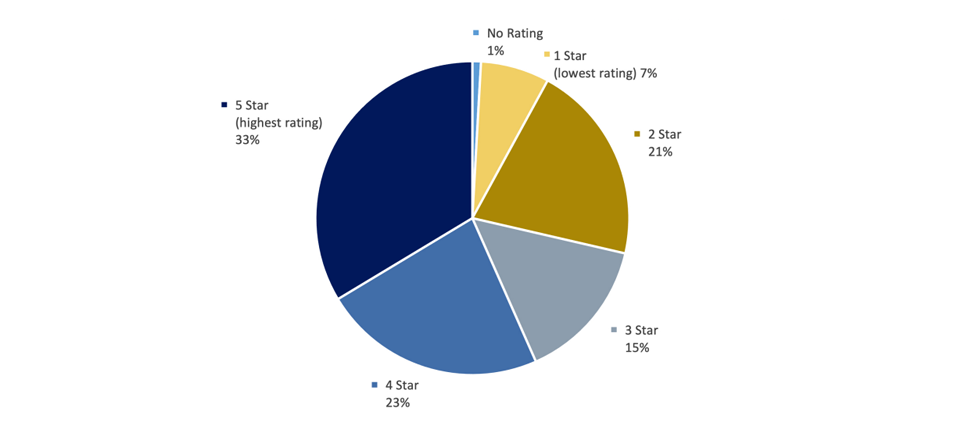
More than half of the 24 LTCs that received one-star as of October 2021 reflected a pattern of several quarters of poor CMS ratings. As one method to evaluate New Jersey’s use of Medicaid funds to pay the lowest-rated LTCs, this report focuses on the LTCs that for the first month of six of the past eight quarters (i.e., January, April, July and October) received one-star. Using this metric, OSC identified 15 LTCs that received one-star on these quarterly intervals for at least six of the prior eight quarters. We refer to these LTCs as the “15 lowest-rated LTCs.”[1] As the Exhibits below show, we analyzed these LTCs not only in terms of their performance on a quarterly basis for the past eight quarters, but also looking back eight years to 2013.
[1] DOH inspection reports for the 15 lowest-rated LTCs, including the examples above, may be found through the DOH links provided for each facility in Exhibit B.
Exhibit B – 15 Lowest-Rated LTCs
| LTC Name | Location | County |
|---|---|---|
| CARE ONE AT EVESHAM CMS Care Compare Page NJ DOH Page |
870 EAST ROUTE 70 MARLTON NJ 08053 |
Burlington |
| CEDAR GROVE RESPIRATORY AND NURSING CENTER (formerly Meadowview Nursing and Respiratory Care - 2019) CMS Care Compare Page NJ DOH Page |
1420 S. BLACK HORSE PIKE WILLIAMSTOWN NJ 08094 |
Gloucester |
| COMPLETE CARE AT FAIR LAWN EDGE (Formerly Complete Care at Passaic County - 2019; Alaris Health at Passaic County - 2017; Riverview Post Acute Care Center - 2013) CMS Care Compare Page NJ DOH Page |
77 EAST 43RD STREET PATERSON NJ 07514 |
Passaic |
| CRANFORD PARK REHABILITATION & HEALTHCARE CENTER (formerly Cranford Hall Nursing Home – 2013) CMS Care Compare Page NJ DOH Page |
600 LINCOLN PARK EAST CRANFORD NJ 07016 |
Union |
| FOREST MANOR HCC CMS Care Compare Page NJ DOH Page |
145 STATE PARK ROAD HOPE NJ 07844 |
Warren |
| LAKEVIEW REHABILITATION AND CARE CENTER (formerly Advanced Care Center at Lakeview - 2015) CMS Care Compare Page NJ DOH Page |
130 TERHUNE DRIVE WAYNE NJ 07470 |
Passaic |
|
NEW GROVE MANOR |
101 NORTH GROVE STREET EAST ORANGE NJ 07017 |
Essex |
| OCEANA REHABILITATION AND NC CMS Care Compare Page NJ DOH Page |
502 ROUTE 9 NORTH CAPE MAY COURT HOUSE NJ 08210 |
Cape May |
| PALACE REHABILITATION AND CARE CENTER CMS Care Compare Page NJ DOH Page |
315 WEST MILL ROAD MAPLE SHADE NJ 08052 |
Burlington |
| RIVERVIEW ESTATES (formerly Baptist Home of South Jersey – 2020) CMS Care Compare Page NJ DOH Page |
303 BANK AVE RIVERTON NJ 08077 |
Burlington |
| SILVER HEALTHCARE CENTER (formerly Alaris Health at Cherry Hill – 2016; Silver Care Health Care Center – 2013) CMS Care Compare Page NJ DOH Page |
1417 BRACE ROAD CHERRY HILL NJ 08034 |
Camden |
| SOUTH JERSEY EXTENDED CARE *SFF (candidate) CMS Care Compare Page NJ DOH Page |
99 MANHEIM AVENUE BRIDGETON NJ 08302 |
Cumberland |
| STERLING MANOR CMS Care Compare Page NJ DOH PAGE |
794 N FORKLANDING ROAD MAPLE SHADE NJ 08052 |
Burlington |
| WARDELL GARDENS AT TINTON FALLS (formerly Liberty Royal Rehab and HCC – 2015) CMS Care Compare Page NJ DOH Page |
524 WARDELL ROAD TINTON FALLS NJ 07753 |
Monmouth |
| WOODLAND BEHAVIORAL AND NURSING CENTER (formerly Andover Subacute and Rehab II - 2020) CMS Care Compare Page NJ DOH Page |
99 MULFORD ROAD ANDOVER NJ 07821 |
Sussex |
|
*LTC identified by the CMS Special Focus Facility Program in January 2021, due to its history of serious quality issues. |
||
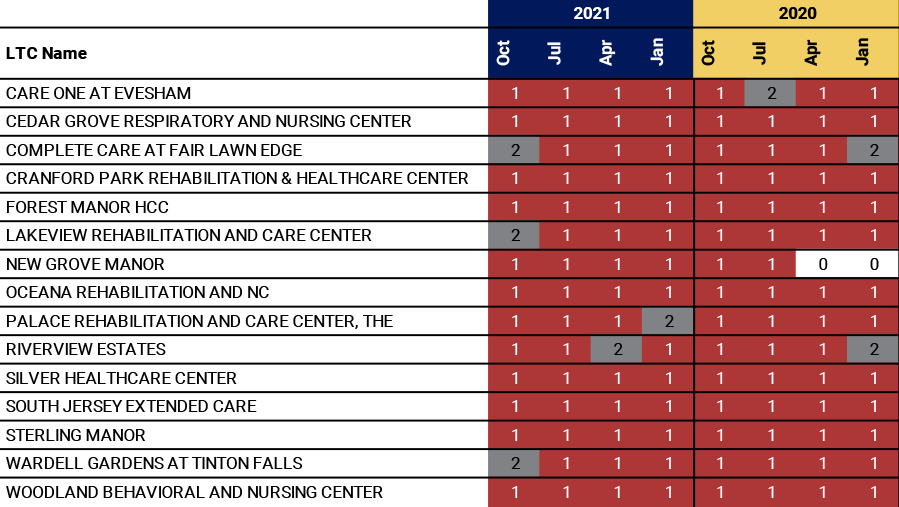
As shown in Exhibit C, these 15 lowest-rated LTCs include 8 that received one-star for all 8 quarterly intervals, 4 that received one-star for 7 out of the 8 quarterly intervals, and 3 that received one-star for 6 out of the 8 quarterly intervals dating back to January 2020.
*LTC received an Overall Rating of zero (0) while in the CMS Special Focus Facility Program.
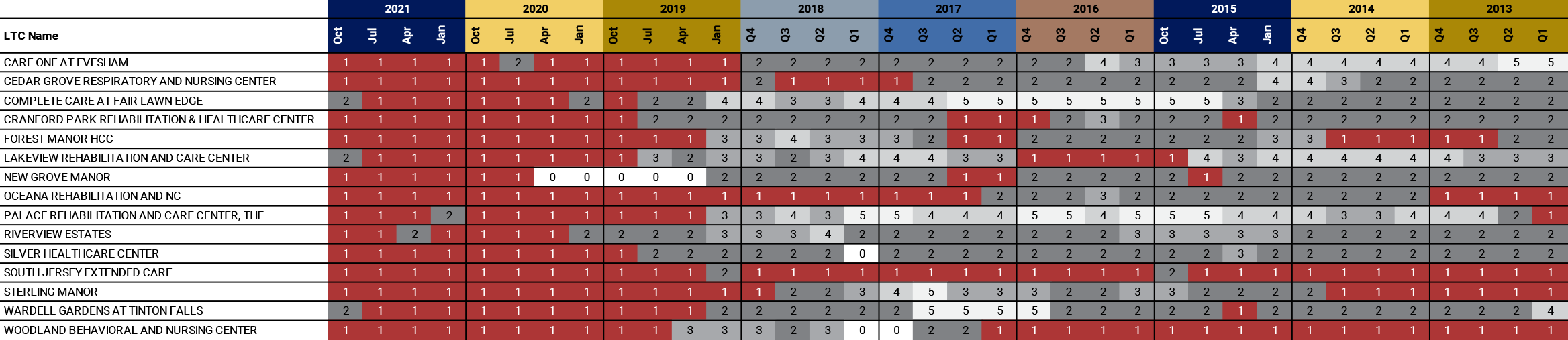
Even more troubling, as shown in Exhibit D, further analysis of these 15 LTCs using the CMS Overall Ratings back to 2013 revealed that many of them have been among the lowest-rated LTCs for many years. Others appear to have generally deteriorated over time and remained low. Some experienced fast and precipitous declines, and have remained among the lowest-rated in recent years.
*LTC received an Overall Rating of zero (0) while in the CMS Special Focus Facility Program.
In sum, the LTCs identified above currently provide low quality care to their residents and many of them have been providing low quality care for an extended period of time, in some cases dating back more than eight years.
B. New Jersey pays on average about $103 million annually to the 15 lowest-rated LTCs.
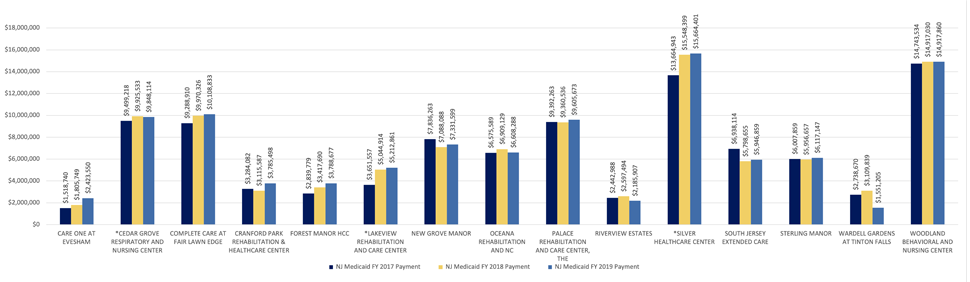
Of the $14 billion spent for Medicaid in fiscal year 2019, Medicaid paid approximately $1.74 billion to LTCs. The 15 lowest-rated LTCs that are the focus of this report together received $105 million in Medicaid funds in state fiscal year 2019, or 6% of the amount that the Medicaid program paid to all LTCs. As shown in Exhibit E below, one of the 15 lowest-rated LTCs received more than $15 million in Medicaid funds both in fiscal year 2018 and in fiscal year 2019.
*LTC is a skilled nursing facility and/or ventilation unit and receives higher per patient reimbursement rates.
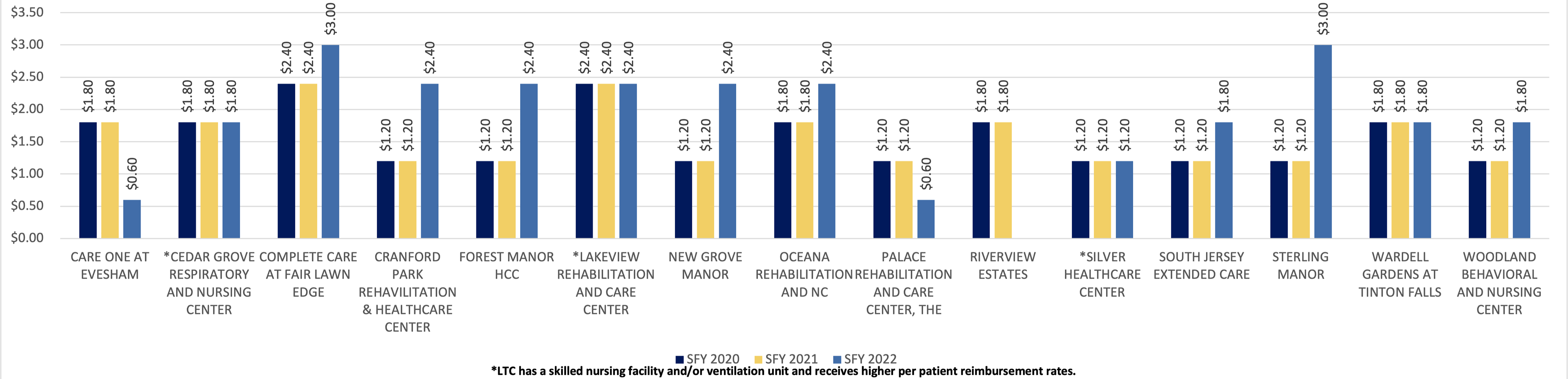
In addition to the payments noted above, beginning in state fiscal year 2020 (July 1, 2019), the Medicaid program, through the Division of Aging Services within DHS, instituted a quality incentive payment program (QIPP) for LTCs. DHS designed the QIPP to provide additional payments to LTCs that demonstrated higher quality/performance. The QIPP measures consider antipsychotic medication use, incidence of pressure ulcers, use of physical restraints, falls with major injury, and CoreQ survey results (a customer satisfaction survey). Through the QIPP, LTCs were eligible to receive an additional $0.60 to $3 per resident per day for meeting or exceeding these five quality measures – a maximum of $0.60 for each measure.[12]
In state fiscal year 2022, the 15 lowest-rated LTCs received an average of $1.97 per resident per day in QIPP payments. The average QIPP payments for all LTCs for this same period was $2.55, just $0.58 more.[13] In addition, despite continuing to receive the lowest one-star rating in state fiscal year 2022, 8 of the 15 lowest-rated LTCs received an increase in SFY 2022 QIPP payments, while 4 maintained the same rate, and only 3 received reduced QIPP payments. See Exhibit F.
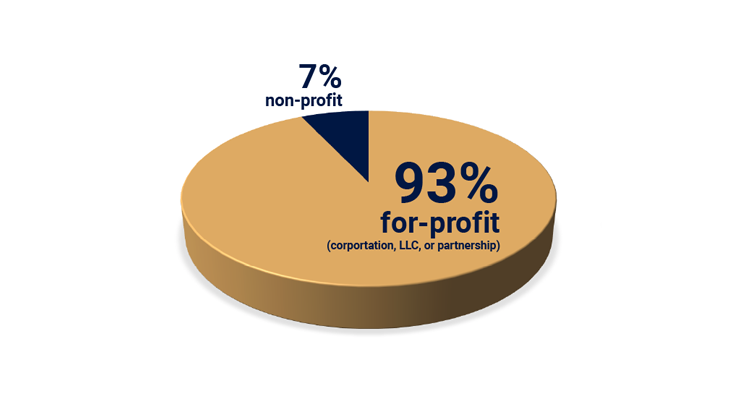
C. 14 of the 15 lowest-rated LTCs are for-profit companies.
Most New Jersey LTCs operate under for-profit ownership models. The vast majority of the 15 lowest-rated LTCs are for-profit organizations, with most operating as a corporation or limited liability company. At least one study has shown that for-profit LTCs increase the short-term mortality risk for patients and lead to declines in other measures of patient well-being, such as lower mobility, while increasing taxpayer costs.[i] Studies have also demonstrated that staffing levels at for-profit LTCs are considerably lower than their government and non-profit counterparts.[ii] There is a strong correlation between overall staffing levels and outcomes, with decreases in staffing leading to worse outcomes, including with regard to mortality.[iii] It is notable that a number of New Jersey LTCs have closed in the past six months and all of these reported closures are not-for-profit facilities.[iv] This trend is worrisome given the above-referenced correlations between outcomes and staffing at these facilities in relation to their for-profit counterparts.
Exhibit G demonstrates the most common organizational structures of the 15 lowest-rated LTCs.
Ownership
We note that of the 15 lowest-rated LTCs listed above, five of the owners/managers/3rd party administrators are also involved in at least two other LTCs on the lowest-rated LTC list. One of these owners/managers/administrators is affiliated with 39 LTCs in New Jersey. Set forth below is a complete breakdown of the affiliations of all five of these owners, managers, and administrators.[18]
- A manager of South Jersey Extended Care, and Sterling Manor, is affiliated with six LTCs that received a two-star or lower score in October 2021 and with a total of nine LTCs in New Jersey
- An owner of Cranford Park Rehabilitation & Health Care Center, Silver Health Care Center, and Wardell Gardens at Tinton Falls, is affiliated with three LTCs that received a two-star or lower score in October 2021 and with a total of five LTCs in New Jersey;
- An owner of Silver Health Care Center, and Wardell Gardens at Tinton Falls, is affiliated with three LTCs that received a two-star or lower score in October 2021 and with a total of three LTCs in New Jersey;
- An administrator of Complete Care at Fair Lawn Edge, Lakeview Rehabilitation and Care Center, Palace Rehabilitation and Care Center, Silver Health Care Center, and Wardell Gardens at Tinton Falls, is affiliated with eight LTCs that received a two-star or lower score in October 2021 and with a total of 39 LTCs in New Jersey; and
- An owner/manager of Oceana Rehabilitation and Nursing Care, South Jersey Extended Care, and Sterling Manor, is affiliated with three LTCs that received a two-star or lower score in October 2021 and with a total of three LTCs in New Jersey.
D. The New Jersey Medicaid program should use its authority to protect current and future residents of LTCs by linking eligibility in the Medicaid program to improvements in ratings.
As noted above, the New Jersey Medicaid program pays LTCs for providing care and boarding to approximately 28,500 beneficiaries, about 6.5% of whom receive care in the 15 lowest-rated LTCs, for which the program pays, on average, $103 million annually. This report urges DMAHS and New Jersey’s policymakers to consider whether New Jersey should demand better quality for the current and future residents of LTCs. That is, should we accept the status quo in which public funds consistently flow to LTCs that, given their history of low ratings, likely will continue to provide below average care? Or, should the Medicaid program use its considerable regulatory authority and spending power in ways that make it less likely that public funds are spent at facilities that provide below-average quality care?
As an entity in state government that is uniquely charged with ensuring that Medicaid funds are used appropriately, OSC urges DMAHS to enact policies that do not permit the state’s lowest-rated LTCs to receive Medicaid funds while remaining well below average for an extended period of time. Although the details of such a policy are best left to DMAHS, and should be integrated with the State’s implementation of other ongoing legislative and regulatory reforms, to convey the concept, we recommend a phased approach that considers the following elements:
- After an LTC receives its first one-star rating: DMAHS provides a warning to the LTC urging the LTC to improve the quality of its care and noting that the receipt of additional one-star ratings may lead to programmatic sanctions. DMAHS could further require the facility to take additional steps, including preparing a corrective action plan to address its deficiencies.
- After two consecutive quarterly one-star ratings (e.g., January and April): DMAHS evaluates whether to impose programmatic sanctions, such as issuing an order barring further Medicaid admissions, capping the total number of Medicaid beneficiaries, and/or reducing or eliminating the LTC’s QIPP payment. In making this determination, DMAHS could consider numerous factors, including patient choice and the availability of LTCs in the relevant geographic region.
- After three consecutive quarterly one-star ratings (e.g., January, April, and July): DMAHS evaluates whether to impose further programmatic sanctions, such as issuing an order barring further admissions, removing existing Medicaid beneficiaries, eliminating QIPP payments, or other measures that protect beneficiaries. In addition, DMAHS, in collaboration with DOH, could further bar owners of the lowest performing LTCs from obtaining interests in or contracting with additional LTCs as a condition of continuing to receive Medicaid funding or by declining to approve an entity’s participation in Medicaid.
If it accepts OSC’s overarching recommendations in this report, DMAHS may follow the methodology above, elect to focus on distinct components of the CMS ratings, or develop its own methodology to establish what constitutes adequate quality of care and how to distinguish between entities that appear likely to improve and those that do not. Whatever metrics, incentives, and consequences are used, the polestar of such a system should be an approach that rejects an outcome that allows Medicaid beneficiaries to be housed in and receive care from LTCs that are perpetually low rated, in favor of one that rewards LTCs that obtain higher ratings and provide high quality care.
DMAHS controls which LTCs may receive Medicaid funds, but does not directly oversee the quality of care the LTCs provide. DOH regulates and evaluates LTCs, but does not control Medicaid funding for LTCs. We recognize that the effective implementation of a policy intended to improve quality of care in LTCs will require the two agencies to carry out their respective duties in ways that take into account and complement the other agency’s efforts.
Implementing policies such as the ones suggested in this report may require the adoption of regulations and the cooperation and support of CMS through State Plan Amendments or other means. But, given the flexibility that the federal government affords states to operate their Medicaid programs in unique ways, implementing the recommendations in this report may be possible under DMAHS’s existing authority.
Recommendations
OSC offers the following recommendations to improve the quality of care offered by LTCs that provide care for Medicaid beneficiaries:
- DMAHS should establish an approach that is the same as or similar to the one proposed in this report that defines a category of the lowest-rated LTCs and, through a phased process, imposes on these LTCs conditions and consequences tied to improving their quality of care.
- DOH should support DMAHS by sharing information regarding its inspections of LTCs and actively provide guidance to DMAHS in its implementation of an approach intended to improve the quality of care provided to Medicaid beneficiaries. Both agencies should be guided by input from the New Jersey’s Long Term Care Ombudsman regarding LTC quality of care issues.
OSC is required by statute to monitor the implementation of its recommendations.[19] OSC will meet those obligations in this matter by updating this report and sharing data on OSC’s LTC Dashboard
[1] The LTCs addressed in this report are long term care (nursing homes) licensed by DOH. This report does not include the following DOH licensed facilities: residential health care facilities, assisted living residences, comprehensive personal care homes, adult day care, assisted living programs, adult family care, pediatric day care, or dementia care homes.
[2] OSC accessed LTC population data for FFS/NF and MLTSS NF from January 2017, 2018 and 2019 to calculate an average number of LTC residents. See NJ DMAHS Long Term Care Population Data: http://www.njfamilycare.org/analytics/LTC_explorer.html. See CMS Care Compare, Nursing Home Provider and Ownership Datasets (October 2021): https://data.cms.gov/provider-data/archived-data/nursing-homes.
[3] OSC downloaded NJ Medicaid payment data from fiscal years 2017, 2018 and 2019 from the NJ Medicaid System/Shared Data Warehouse and combined Medicaid claims payment data for both Fee for Service and Managed Care Organizations for total payment amounts. The amounts provided are estimates/averages and do not account for future claim edits and/or retractions.
[4] See NJ FamilyCare Total Enrollment: http://www.njfamilycare.org/analytics/home.html.
[5] See NJ Legislature Analysis of DHS Budget, State Fiscal Year 2018-2019: https://www.njleg.state.nj.us/legislativepub/budget_2019/DHS_analysis_2019.pdf.
[6]See CMS Nursing Home, Care Compare Technical Details: https://data.cms.gov/provider-data/topics/nursing-homes/technical-details.
[7] See Abt Associates, Nursing Home Compare Five-Star Quality Rating System: Year Five Report, Figure 3.1a, June 16, 2014: https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/CertificationandComplianc/Downloads/NHC-Year-Five-Report.pdf.
[8] See Abt Associates, Nursing Home Compare Five-Star Quality Rating System: Year Five Report, Figures 3.1b and 3.1c, June 16, 2014: https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/CertificationandComplianc/Downloads/NHC-Year-Five-Report.pdf.
[9] See CMS Care Compare Technical Users’ Guide: https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/CertificationandComplianc/downloads/usersguide.pdf.
[10] See DOH Scope and Severity Definitions (accessed November 4, 2021) (emphasis added): https://healthapps.state.nj.us/facilities/fsSs.htm
[11] See CMS Care Compare, Nursing Home Provider and Ownership Datasets: https://data.cms.gov/provider-data/archived-data/nursing-homes.
[i] DOH inspection reports for the 15 lowest-rated LTCs, including the examples above, may be found through the DOH links provided for each facility in Exhibit B.
[12] See Nursing Facility Quality Incentive Payment Program presentation from October 2019: https://www.state.nj.us/humanservices/doas/documents/NF%20Quality%20Incentive%20Payment%20Program%20October%202019%20Final.pdf.
[13]See SFY 2022 Nursing Home Rate File: https://www.nj.gov/humanservices/doas/documents/NH%20Rate%20Worksheet%20SFY%202021-22-KS%20091021-%20website-%20R1.1.6-R1.pdf.
[14] See National Bureau of Economic Research Working Paper, DOES PRIVATE EQUITY INVESTMENT IN HEALTHCARE BENEFIT PATIENTS? EVIDENCE FROM NURSING HOMES, February 2021: https://www.nber.org/system/files/working_papers/w28474/w28474.pdf.
[15] See Abt Associates, Nursing Home Compare Five-Star Quality Rating System: Year Five Report, Figures 3.2, June 16, 2014: https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/CertificationandComplianc/Downloads/NHC-Year-Five-Report.pdf.
[16] See National Bureau of Economic Research Working Paper, DOES PRIVATE EQUITY INVESTMENT IN HEALTHCARE BENEFIT PATIENTS? EVIDENCE FROM NURSING HOMES, February 2021: https://www.nber.org/system/files/working_papers/w28474/w28474.pdf (30-31).
[17] See NJ Spotlight, Two nursing homes close and may signal a trend, May 10, 2021: https://www.njspotlight.com/2021/05/two-nursing-homes-close-and-may-signal-a-trend/; NJ.com, More nursing homes and senior living facilities are closing their doors because of COVID’s impact, July 12, 2021: https://www.nj.com/coronavirus/2021/07/more-nursing-homes-and-senior-living-facilities-are-closing-their-doors-because-of-covids-impact.html; and NorthJersey.com, Bergen County to permanently close Rockleigh nursing home in wake of COVID pandemic, July 16, 2021: https://www.northjersey.com/story/news/health/2021/07/16/bergen-county-health-care-center-closing-nj-covid/7991813002/.
[18] See CMS Care Compare, Nursing Home Provider and Ownership Datasets (October 2021): https://data.cms.gov/provider-data/archived-data/nursing-homes.
[19] See N.J.S.A. 52:15B-15; N.J.S.A. 52:15C-11a; N.J.S.A. 30:4D-60b.
Waste or Abuse
Report Fraud
Waste or Abuse
 Official Site of The State of New Jersey
Official Site of The State of New Jersey